Portal User Manual – Prior Authorization
You currently have jurisdiction selected, however this page only applies to these jurisdiction(s): .
Print the complete Portal User Manual ![]()
CMS established a prior authorization (PA) program for a limited number of services. For Medicare Part A, the PA program applies only to the following services when they are performed in a hospital outpatient department (HOPD) and submitted on a 13x type of bill:
- Blepharoplasty
- Botulinum toxin injections
- Cervical fusion with disc removal
- Facet Joint Interventions
- Implanted spinal neurostimulators
- Panniculectomy
- Rhinoplasty
- Vein ablation
See Prior Authorization for Hospital Outpatient Department Services (HOPD) Overview for an overview of the process. (You will need to select J5A or J8A at the top of the page to view the full article.)
CMS established a PA program for Medicare Part B Repetitive, Scheduled Non-Emergent Ambulance Transport (RSNAT). Procedure codes for the RSNAT program are:
- A0426 - Ambulance service, advanced life support, non-emergency transport, level 1 (ALS1)
- A0428 - Ambulance service, basic life support (BLS), non-emergency transport
- Associated Service A0425 - Ground mileage, per statute mile
Procedure codes A0426 and A0428 require prior authorization; A0425 does not require prior authorization.
See Prior Authorization for Repetitive, Scheduled Non-Emergent Ambulance Transport (RSNAT) for more information. (You will need to select J5B or J8B at the top of the page to view the full article.)
Submitting a Prior Authorization Request
HOPDs and Ambulance Suppliers can use the WPS Government Health Administrators Portal to submit PA requests and supporting documentation to our Medical Review department. To access the Prior Authorization area of the portal, click on the Prior Authorization link under the My Correspondence heading in the left navigation menu.

For OPD Prior Authorization Requests:
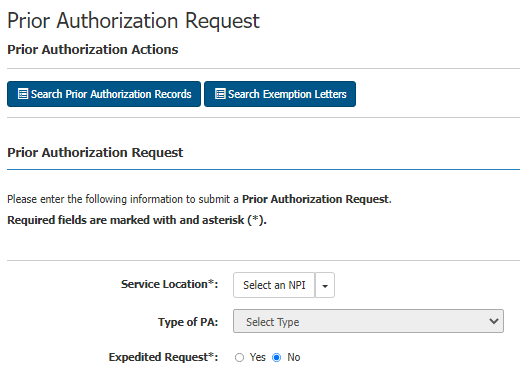
Step 1: Begin by selecting the NPI service location for the facility. Select the type of service you are providing from the drop-down box. Also, select the appropriate radio button to indicate whether the request needs to be expedited. Providers may only submit expedited requests if the standard timeframe for making a decision could seriously jeopardize the life or health of the patient.
NOTE: If the supplier or facility’s NPI does not appear in the drop-down list, you will need to request access to the NPI under My Service Locations before submitting your prior authorization request through the portal.
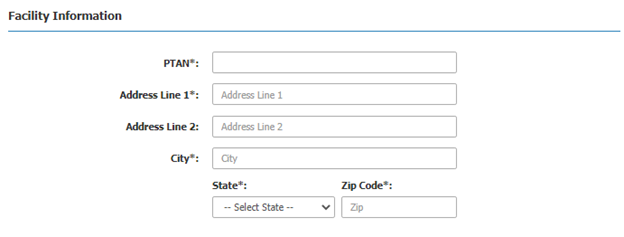
Step 2: Next, enter the PTAN and address for the facility where the service will be performed.
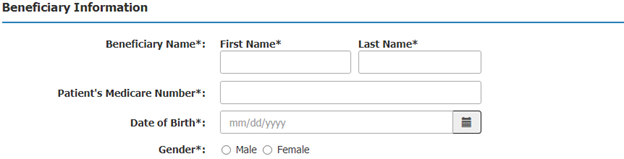
Step 3: Enter the patient’s name, Medicare number, date of birth, and gender.
Step 4: Enter the requester’s name, title, and contact information.

Step 5: Enter the physician/practitioner’s name, NPI, PTAN, and address.
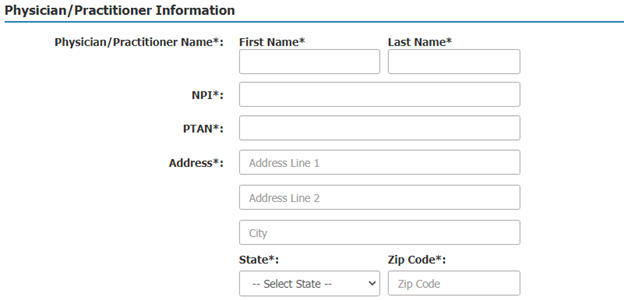
Step 6: Enter details about the procedure that will be performed, including the anticipated date of service, procedure code (CPT or HCPCS code), modifiers, and any additional pertinent information.
NOTE: If approved, the prior authorization is valid for 120 days. If the actual date of service will differ from the anticipated date of service, you do not need to submit a new request if the procedure is performed within 120 days of the prior authorization decision.
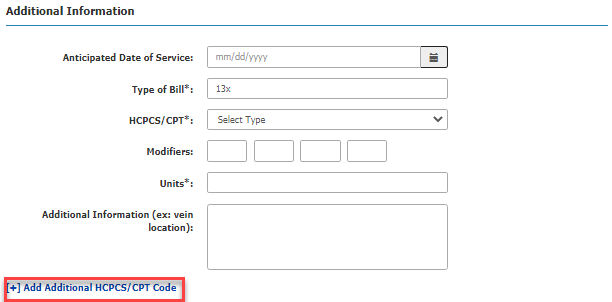
NOTE: If the provider will be performing more than one procedure that requires prior authorization, or if the provider may change the procedure intraoperatively, click the “Add Additional HCPCS/CPT Code” link to provide information about the additional procedures. It may be best to submit a prior authorization request with several potential service codes to avoid a claim denial due to no prior authorization.
Step 7: Upload documentation that supports the medical necessity for the procedure(s). Click the “More Information” link (also located near the top of the page) to see the documentation that should be provided for each type of service.
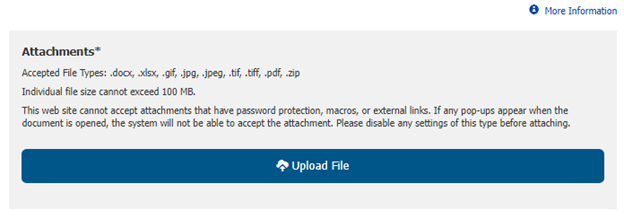
Documentation cannot be password protected, contain macros, or have external links. We accept documentation in the following file formats:
- .tif
- .tiff
- .doc
- .docx
- .xls
- .xlsx
- .jpg
- .jpeg
- .gif
- .zip
The uploaded file must be smaller than 100 MB. If you need attach multiple files, you must put them into a single .zip file containing no more than 60 individual files. The files in the .zip file must be in one of the formats listed above.
Step 8: After entering the required information and uploading the supporting documentation, click the Continue button at the bottom of the page. Correct any errors, then click Submit to submit your prior authorization request to Medicare. If your submission is successful, you will see a confirmation page containing a confirmation number.
For RSNAT Prior Authorization Requests:
Step 1: Begin by selecting the NPI service location for the facility. Select the type of service you are providing from the drop-down box. Repetitive, Scheduled Non-Emergent Ambulance Transport will be selected. Select the appropriate radio button to indicate whether the request needs to be expedited. Providers may only submit expedited requests if the standard timeframe for making a decision could seriously jeopardize the life or health of the patient.
NOTE: If the supplier or facility’s NPI does not appear in the drop-down list, you will need to request access to the NPI under My Service Locations before submitting your prior authorization request through the portal.
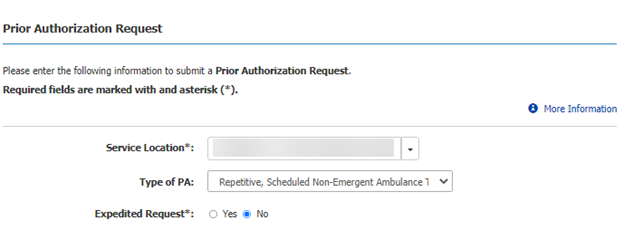
Step 2: In the Supplier Information section, enter the PTAN and address. Select the state where the ambulance is garaged,
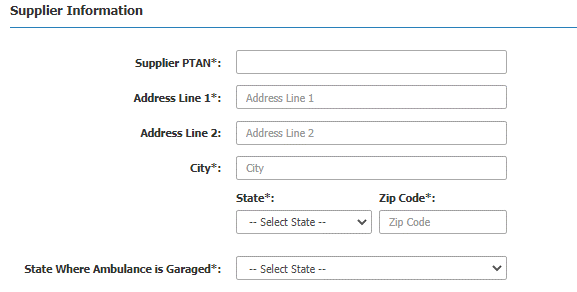
Step 3: Enter the patient’s name, Medicare number, date of birth, and gender.
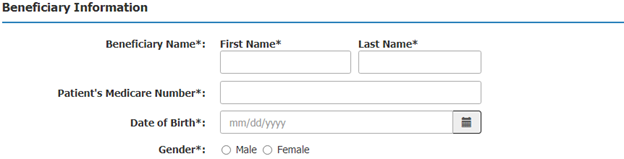
Step 4: Enter the Requester and Contact information.
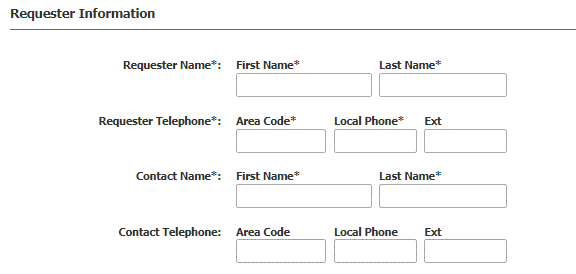
Step 5: Enter the Certifying Physician information
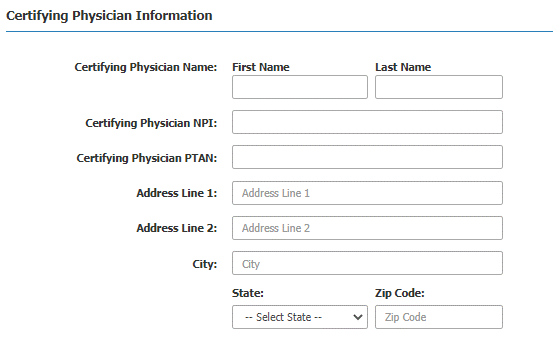
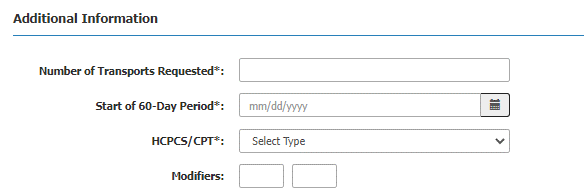
Step 6:
Enter the number of transports requested, start of the 60-day period, select the HCPCS, modifiers are optional.
Step 7: Upload documentation that supports the medical necessity for the procedure(s). Click the “More Information” link (also located near the top of the page) to see the documentation that should be provided for each type of service.
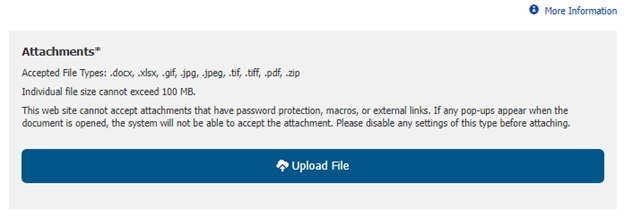
Documentation cannot be password protected, contain macros, or have external links. We accept documentation in the following file formats:
- .tif
- .tiff
- .doc
- .docx
- .xls
- .xlsx
- .jpg
- .jpeg
- .gif
- .zip
The uploaded file must be smaller than 100 MB. If you need to attach multiple files, you must put them into a single .zip file containing no more than 60 individual files. The files in the .zip file must be in one of the formats listed above.
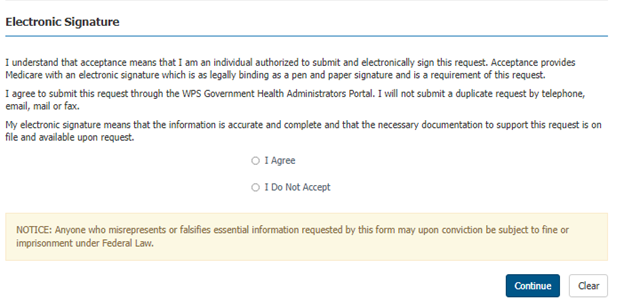
Step 8: You must provide an electronic signature by marking I Agree. If you do not accept, you will not be able to submit the Prior Authorization in the portal.
Step 9: After entering the required information and uploading the supporting documentation, click the Continue button at the bottom of the page. Correct any errors, then click Submit to submit your prior authorization request to Medicare. If your submission is successful, you will see a confirmation page containing a confirmation number.
Searching for Prior Authorization Requests and Decisions
After submitting a prior authorization request through the portal, you can monitor its status and view the decision letter within the portal. Begin by clicking on the Prior Authorization link in the left navigation menu to enter the Prior Authorization section of the portal. Click the Search Prior Authorization Records button at the top of the page to begin the search.
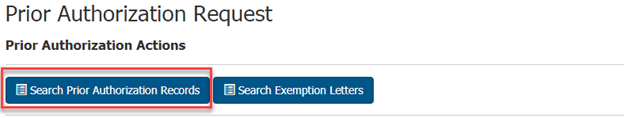
This will show a table containing all the prior authorization requests you are able to view. You can click the column headings to sort the results by that column. You can also narrow the results to see only a certain type of prior authorization or only those requests you submitted yourself. You can also use the filter to search for specific information in the table, such as a specific Medicare number. Click on the Confirmation Number to view a record.
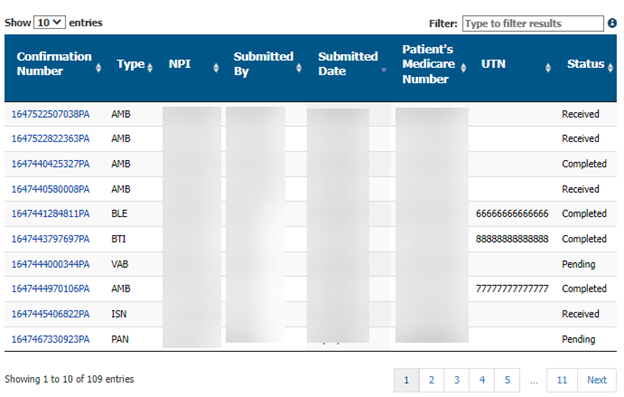
Status Codes:
Received – The attachment has been submitted and is waiting for virus scanning.
Pending – The request has been received by the Medical Review department.
Completed – A decision letter is available to view.
Not Accepted – The file was invalid or corrupt. Review the accepted file types and resubmit.
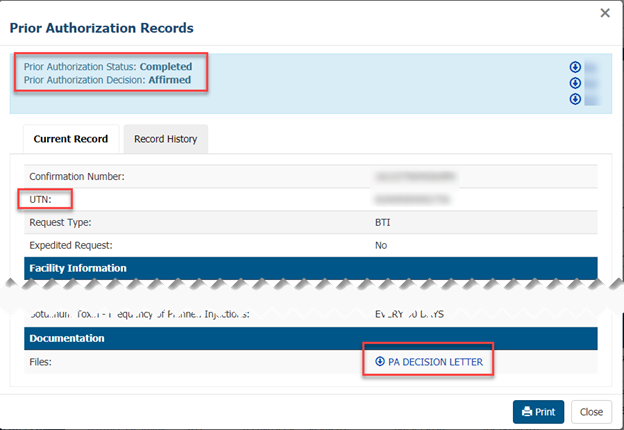
Once you open a record, you will find:
- The status of the request and the prior authorization decision at the top of the record
- The details of the request (on the Current Record tab)
- The Unique Tracking Number (UTN) (if the request is affirmed or non-affirmed)
- The decision letter that provides full details about the completed request (affirmed, non-affirmed, or rejected)
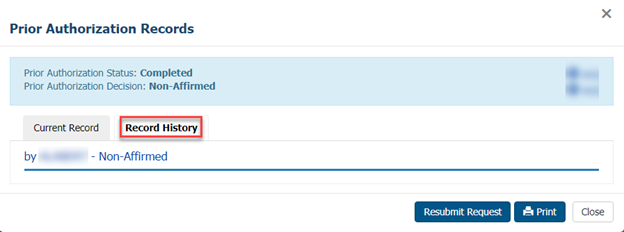
Subsequent Requests
If the request is non-affirmed, you can resubmit the request to provide additional information. Click the Resubmit Request button at the bottom of the page, which will open the prior authorization request form prepopulated with the details from the previous request.
NOTE: You will not see the Resubmit Request button if the decision is affirmed or rejected.

The Record History tab will show the history of your previous requests.
Searching for Prior Authorization Exemption Letters
CMS has the authority to exempt a provider from the prior authorization process if the provider demonstrates compliance with Medicare coverage, coding, and payment requirements. CMS also has the authority to withdraw such an exemption. WPS Government Health Administrators will notify a provider by letter if they are exempt from the prior authorization process or if their exemption is withdrawn. Providers can locate their exemption letters in the portal by clicking on the Search Exemption Letters button.
Click on the View Letter button to see the letter. You can also sort the letters by letter type or filter the results to find a specific letter.